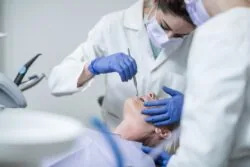
Dental Implant Health Assessment: Understanding the use of probing
Former President of the BSDHT, Michaela O’Neill, talks us through the steps Dental Hygienists and Therapists need to take when assessing the health of their patients’ implants.
The rise of dental implants has been one of the most significant changes in our patients’ dentitions in the past 10 years. What used to be a rarity, is now a much more mainstream procedure among patients.
This increase is opening doors for Dental Hygienists and Therapists, who are responsible for maintaining good oral health post implant. Our role is to recognise and diagnose any signs of periodontal diseases early on, so we can properly care for and treat our patients.
To demonstrate the best practice behind looking after and managing dental implants, I have created a simple guide to carrying out your implant health assessments using dental probing.
Risk to dental implants
There are several contributors to peri-implant diseases, but bacteria is one of the largest causes.
Implants are vulnerable to bacterial plaque, which can cause an inflammatory response in the peri-implant tissues. This is because there is a strong cause-effect relationship between dental plaque and peri-implant diseases.
With diseases like peri-mucositis and peri-implantitis so common in patients with dental implants, regular health assessments are crucial in helping patients maintain good oral health. So, what is involved in a best practice implant health assessment?
To probe, or not to probe?
There is much debate about best practice when it comes to assessing the health of our patients’ implants, with some professionals siding for probing, while others argue against this technique.
However, the Consensus Report of the Sixth European Workshop on Periodontology concluded that “Probing is essential for diagnosis of peri-implant diseases”. The reports states that, to evaluate the presence of health or peri-implant disease, we must record:
- Bleeding on probing
- Suppuration
- Probing depth
- Radiographic bone loss
- Implant mobility
These are insights that can only be gathered when using a probe. Something that the 11th European Workshop on Periodontology further supported.
“Bleeding on probing is considered a key clinical measure to distinguish between peri-implant health and disease.”
11th European Workshop on Periodontology
As the tissues surrounding implants are not connected to the implant’s surface in the same way as the tissues around teeth are attached, they are less resistant to probing.
The position of the implant, in relation to the bone and soft tissues, may also lead to deeper probing depths when compared to healthy tissues. This is why the Basic Periodontal Examination (BPE) is not an appropriate approach to the assessment of implants.
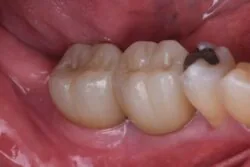
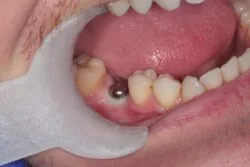
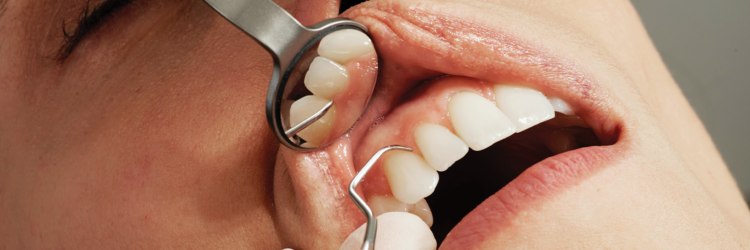
How to probe a dental implant
When it comes to probing a dental implant, look out for the following:
- The loss of crestal bone can be a key indicator that peri-implantitis is present.
- There may be pocket depths from the surgically created sulcus, rather than from development.
- Suppuration is quite common, and not necessarily a sign of active disease.
If longer implant abutments have been used, you will often have to probe further to properly assess the state of the tooth.
One of the most important aspects of assessing implant health is being able to compare change over time. This is why you should always encourage regular maintenance visits from your implant patients. When you carry out an assessment, ensure you record findings clearly, including pocket depths, bleeding and suppuration.
The only time you should avoid probing a dental implant is during the initial healing and integration phase. This time will vary depending on which dental professional placed them. It is up to you to find this information out.
“Whilst probing is crucial for detection of disease, don’t forget to assess and record tissue health visually. Recording the location of these changes (e.g., lingual or interproximal) helps to individualise and focus oral hygiene instruction.”
British Society of Periodontology
Choosing an implant probe
Implants must be measured with a calibrated probe, not a World Health Organisation (WHO) probe. The general consensus is that a metal or plastic probe may be used, however flexibility is important as it allows you to follow the anatomy for an accurate clinical reading.
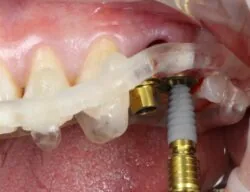
One of the major obstacles to probing can be the superstructure. Compared to the neck of the implant, the restoration can be quite bulbous and difficult to circumnavigate in order to allow the probe to enter a pocket. The disadvantage of less flexible materials is that they can be difficult to position for an accurate pocket depth. Getting around this requires a degree of flexibility in the probe.
This is why the Deppeler PP12 implant probe is the tool of choice for many clinicians familiar with implants. Made of PEEK plastic, this probe’s flexibility offers improved accuracy when navigating superstructures. It also delivers enough firmness, which allows you to slide over the implant rungs and reach the base of the pocket. The Deppeler also benefits from black band markings at 3, 6, 9, and 12mm, which are abrasion resistant for long lasting results.
For further information on how BioHorizons Camlog can support hygienists and therapists in the role of implant dentistry check out our education programme.