Case Study: Bone augmentation of a large cyst and defect
Dr Devang Patel presents a bone grafting procedure carried out using MinerOss® allograft material to augment a large defect. Read the full case study to understand his approach to both the bone augmentation and implant placement surgery.
Patient presentation
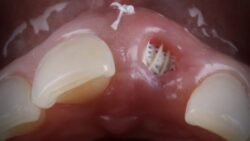
The patient presented with large radicular cyst associated with UR1 and UR2. UR1 was fractured and discoloured whereas UR2 had large root resorption and hence had to be extracted.
Teeth were extracted and cyst enucleation was carried out. You can see the root exposure of UR3 due to extent of the cyst. Biopsy was sent to identify the cyst.
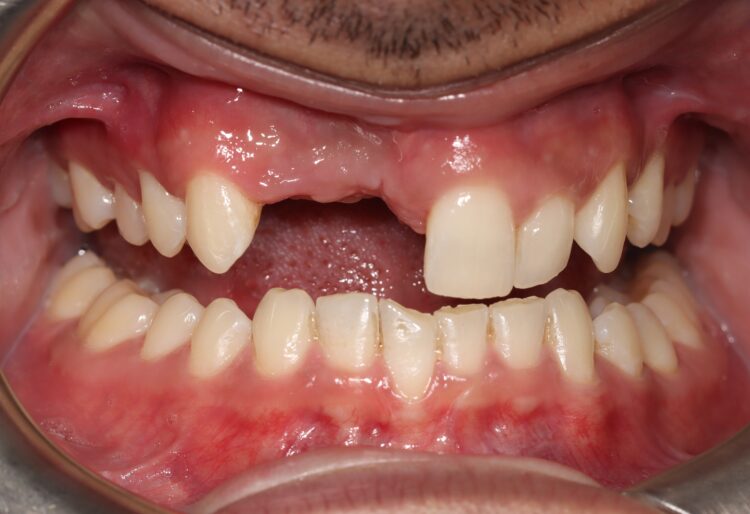
Figures 1, 2 and 3 shows pre–op situation and the defect after cyst removal on the day of the surgery.
The wound was closed and allowed to heal for 3 months. No bone grafting was used at this stage as we were waiting for the pathology report before any grafting.
Figures 4 and 5 show post-healing defect.
Treatment options
Post-healing following treatment options were discussed:
- Leave the space as it is – however this is not realistic due to the position of missing teeth.
- Partial denture – Patient declined this option and wanted a fixed option.
- Implant restorations – We informed the patient that he would need a two-stage approach where we will have to augment the bone first and then re-enter after a certain time to place the implants.
Various bone grafting materials were discussed including autogenous grafting, using xenograft or allograft. To give the best outcome, we decided to go with the option of allograft mixed with autogenous bone scrapings.
Surgery 1: Bone augmentation
During surgery, the area was exposed. As you can see some of the defect had already filled with host bone (fig. 6).
MinerOss allograft block was sectioned and used as a plate and MinerOss cortical cancellous bone was used with 60% autogenous / 40% MinerOss mixture between the plate and host bone. Autogenous bone was harvested from the oblique ridge area. Instead of harvesting a block and crushing the block, on this occasion we decided to scrape particulate bone and collect it as the patient had an impacted third molar and harvesting a block could have risked exposing a molar and needing unnecessary removal.
Stoma 1.0mm stainless steel screws were used to secure the allograft plate at a suitable distance. The area was closed passively using 5-0 and 6-0 glycolon sutures.
Surgery 2: Implant placement
Six months after bone augmentation surgery, the area was exposed and a very good quality vascular bone was found. This was well integrated so we could remove the screws and place the implant without destabilising the plates.
CONELOG® implants from BioHorizons Camlog were placed subcrestal and palatally. It is vital to note that autograft and allograft bone may resorb to stay within the contour of the actual bone morphology of the patient, hence it is very important to consider this while placing implants.
Conclusion
The Khoury technique, using autogenous bone plates with autogenous particulate bone between the plates, is considered gold standard for bone grafting. However, in my opinion, when it is not possible to harvest large autogenous bone, or if the surgeon and patient would like to reduce the morbidity of the procedure, then this technique of using allograft bone graft material mixed with autograft material can provide a perfect solution.
The advantage of this technique is that no block harvesting is needed, which reduces the patient morbidity and large bone grafting can be carried out. However, in my opinion, it is still best to use 60% of the autogenous bone grafting material to be mixed with allograft to give the best success, so it does not completely avoid a second harvesting site.
This procedure could have been performed using an allograft and autograft mixture stabilised using a titanium membrane; however in this case plates from the allograft block were used to stabilise the bone particles and autogenous bone chips.
“When mixed with autogenous bone graft, allograft material can give an amazing result. In my opinion, bone quality is as good as pure autogenous bone graft if not better. I would recommend MinerOss allograft material.”