Single implant placement with GBR.
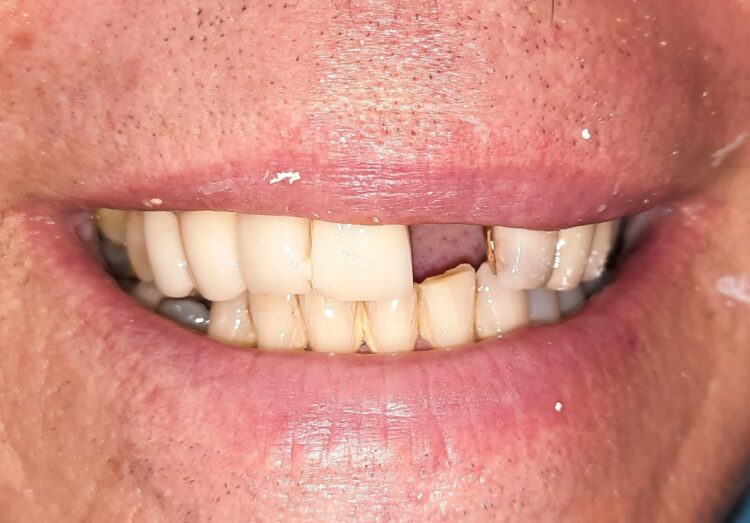
Single implant placement with GBR
Dr Jonathan Dougherty discusses an anterior implant placement with GBR using the CONELOG® PROGRESSIVE-LINE implant.
Patient presented for implant placement
This medically fit, 64-year-old male, who was a non-smoker and a regular attender, presented with a fractured UL1. The patient previously had a crown in place however on presentation it was evident that the crown had fractured, and a retained root was present. Whilst the patient had a stable dentition with good posterior support, they presented with a thick gingival biotype and low smile line with low aesthetic demands. This was assessed via a patient physiological questionnaire which is part of my initial consultation proforma.
Treatment options
We discussed various clinical treatment options with the patient, but their main concern was to restore the space without damaging any of the adjacent teeth.
It was evident that the long-term prognosis of the UL1 was poor, however we discussed various clinical treatment options with the patient.
Option 1 – The possibility of root canal treatment and the provision of a post core and crown.
Option 2 – Remove the root and provide a denture, made from either acrylic in the immediate term with a view to providing either cobalt chrome, or a conventional fixed bridge long term.
Option 3 – Removing the retained root and providing a dental implant with a view to providing an implant retained crown.
The patient did not want to proceed with a denture as he wanted something secure so that he could eat comfortably. He also chose not to have a bridge as he did not want to damage his front teeth any more than they had been, as they were already restored with veneers.
It was agreed that an implant with a single crown would be the best option for the patient as it would mean we could provide a fixed long-term option without damaging his adjacent teeth. We are aware that 20% of teeth which have had a crown preparation can require root canal treatment after five years and this is something the patient wished to avoid if possible. Thus, a dental implant was the best choice.
Treatment process
As always a thorough examination protocol was followed. We have a checklist proforma which is completed throughout the consultation process. This ensures we collect all the information we need to assess the case in a methodical manner, and also allows me to risk assess the case.
Once we completed our intraoral exam we provided the patient with a wax up to gain aesthetic approval. It’s vital to plan via a restorative approach so that we can place the dental implant in the correct position and therefore provide a predictable restorative outcome for both the patient and clinician alike. Failure to do so, could result in a compromised restorative outcome and an unhappy patient.
We confirmed aesthetics via our wax up and thus proceeded to take a CBCT with the patient wearing an essix retainer containing a radiopaque tooth based on the agreed wax up. We then selected the appropriate width and height of the implant based on bone volume availability. Thorough examination showed positive bone availability for the placement of a CONELOG® PROGRESSIVE-LINE implant (3.8x 11mm).
However, during the surgical appointment the buccal plate fractured during root removal and as such we had to adapt our proposed plan. I raised a 2-sided full thickness flap and was able to place the implant as planned. It was evident however that a graft was required. I used a mixture of Auto/Xenograft and a membrane to cover the graft material. I then placed layered sutures starting with horizontal mattress sutures to secure the membrane and multiple interrupted sutures to secure the flap. I used 4.0 Vicryl Rapide Sutures.
The result
All implant planning should be restoratively driven, and a comprehensive treatment plan is key for any successful surgical outcome.
However, sometimes things do not go according to plan and this case is a good example of that. In scenarios like this, it’s essential not to panic and instead to follow the basic principles. With this premise, I managed to achieve good primary stability of the implant plus we had a 3 walled defect, thus we could predictably graft this site and still achieve a suitable outcome for the patient.
For more information about the CONELOG® PROGRESSIVE-LINE implant click here. Or to read more articles from Jonathan Dougherty click here.



















