Offering quality full-arch implant treatment in a timely fashion

David Murnaghan offers insight into a full-arch implant case using TeethXpress, meeting both the patient’s expectations and best practice implant protocols, to achieve an outstanding outcome.
Case presentation
This 69-year-old female patient presented to the practice as a very nervous patient and had lapsed from attending any dental practice over long periods. A smoker, she presented with a failed upper dentition and many failing lower teeth. Unfortunately, following initial assessment, it was determined that the upper teeth had a hopeless prognosis and required a full clearance. Some of the lower teeth also required removal and this was carried out alongside rigorous periodontal treatment.
Quality of life and success depend greatly on patients’ expectations and vary dramatically in differing populations (McGrath and Bedi, 2002; 2003). Today, people expect the dental profession to be able to provide restorations beyond dentures. Dentists, therefore, have to try either to live up to and deliver patients’ expectations or explain why it is not possible while keeping them happy.
Of course, it is not possible to keep everyone happy all of the time, and it can be a balancing act when ensuring we are not risking treatment that could be detrimental to a patient’s health or dentition.
Possible treatment options for this patient following a full upper clearance were:
- A full upper denture
- An implant-retained denture
- Four implants with precision attachments or a bar with a full denture as an interim prosthesis
- Fixed teeth:
- Six to eight implants alongside a sinus lift with a delayed approach using a full denture as an interim prosthesis
- Four implants designed to allow immediate loading, if the implants could be adequately retained with 35 Ncm torque in the bone, or delayed restoration with an interim full denture.
The patient was very clear from the outset that she wanted to avoid removable teeth, if possible. Fixed teeth, of course, have the disadvantages of being more complicated to keep clean and more expensive, but the advantages of increased comfort, confidence and quality of life.
The patient was advised that she had to stop smoking and show commitment in the form of several hour-long periodontal appointments with the hygienist before a fixed option could be considered. The patient showed the necessary commitment, after which a higher risk option of TeethXpress was discussed; namely, extracting all the teeth that needed to be removed, placing all the implants in strategic positions, and fixing a prosthesis screwed into place in a single day.
How many implants?
Traditionally, a minimum of five or six implants would be placed to restore a fixed arch. An alternative, recognised treatment plan originally designed by Paulo Malo, which uses straight and angled multi-unit abutments with only four implants has been widely used now for around 25 years.
The biomechanics of this treatment indicate that the most important factor is not the number of implants but the anterior-posterior (AP) spread of implants (Belivacqua, 2011). Studies have indicated that four versus five implants show no increase in success or reduce complications. It has been said that you can have four but not three; therefore, it is more prudent to place five implants for security. However, a lot of the time, if an implant fails when five were originally placed, it will not act like a multi-unit abutment with four implants. This is because the implants will not be in the same strategic position and therefore it will be no better than an ‘all-on-3’ (Brunski, 2014).
Choosing the best option
When choosing a prosthetic solution, there are several pertinent decisions to be made:
- Screw access trajectory – ideal vs. non-ideal
- Restorative space – acrylic vs. ceramic
- Opposing occlusion – natural, denture or implant
- Arch – maxilla or mandible
- Force – high or low
- Aesthetic demand – high or low
- Cost
As the screw access trajectory would not be ideal in this case, multi-unit abutments would be needed to ensure a screw-retained prosthesis and space would need to be created to allow for this. An acrylic superstructure was decided upon, to ensure good aesthetics of the ‘pink and white’ while also considering financial factors with the patient. The opposing dentition was mixed restoratively and therefore suitable for the less abrasive acrylic. Forces were judged to be moderate from the failed dentition’s mild tooth wear.
The treatment
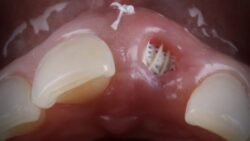
Two months later, following smoking cessation, extensive oral hygiene instructions and periodontal treatment, all of the patient’s upper teeth were removed. The sockets were debrided and all granulation tissue removed to ensure only healthy bone remained.
Distal implants (BioHorizons Tapered Internal Laser-Lok 4.6mm | 12mm) were strategically used following planning from a CBCT scan to utilise anterior-posterior spread and avoid the sinuses. Anterior implants (BioHorizons Tapered Internal Laser-Lok 3.8mm | 12mm) were placed at the apex of the original teeth (following bone reduction), utilising deeper bone and creating space for the restorative components. To improve the emergence profile of the implants, 17-degree multi-unit abutments were torqued at 35 Ncm. Titanium cylinders were then fitted at 15 Ncm to engage an acrylic denture.
Dental technician, Michael Allison of Gordon Watters Laboratory, attended on the same day and assisted with the pickup of the acrylic denture and reformation of it to a neater, more comfortable prosthesis. The fixed denture was torqued at 15 Ncm, screw access holes were protected by PTFE tape and sealed with Fuji IX.
The patient was instructed to stick to a soft diet for two months and to use chlorhexidine-based PerioKin gel and Kin Gingival mouthwash to assist with antibacterial cleaning. The patient was then left to heal for two weeks, after which at the sutures were removed and the healing process checked. This was left for a further three months, to allow for further healing and osseointegration to take effect.
Following three months of osseointegration, impressions were taken of the existing bridge in situ, as well as a special tray open tray impression with Hereaus Kulzer putty, plus a wash impression of the multi-unit copings.
The patient was restored definitively five months after treatment and attended the hygienist every three months since placement. The bridge will be removed annually for a deep clean by the hygienist. In between appointments, the patient uses a Waterpik Complete Flosser twice-daily to clean effectively.
The patient has reported greatly improved comfort during function, and her confidence has increased dramatically.
TeethXpress is a biomechanically-stable, immediate load and function protocol for fully- or partially-edentulous patients. BioHorizons Tapered Implants with Laser-Lok technology provide superior primary stability for immediate load. For more information about full-arch rehabilitation with TeethXpress, visit theimplantrevolution.co.uk.