Complete your implant practice with full arch treatment
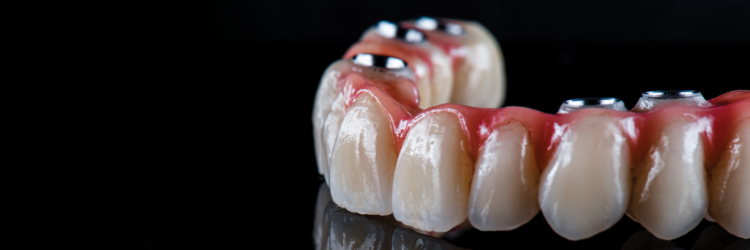
Full-arch implants, including single-day procedures and implant-retained dentures are in hot demand right now, as patients become increasingly aware of the benefits these rehabilitative solutions can offer them. Suitable for patients with a failing dentition, advancements in full arch treatment mean that we are now able to combine extraction, placement of between 4 and 6 fixtures and abutments and the delivery of a fixed bridge within a single day.
Immediate full-arch restoration in a day is a paradigm shift compared to the more traditional conventional methods for large restorations that were carried out in the past. Although it seems complex, with careful planning and the right team it can be life-changing for patients. For any clinician considering becoming involved in full-arch rehabilitation, there are three important skill types to grasp; surgical, restorative and communication skills, as they will assist in understanding how to attract suitable patients, when to treat them and when to refer.
Screw-retained hybrid – yes or no?
Classed as an FP3 (fixed prosthetic), where a fixed prosthetic combines teeth and gums to deliver a hybrid restoration, we’re not just looking at replacing the hard tissue, but the soft tissues too. A screw-retained hybrid allows patients to have teeth immediately – if we replace the lost hardened soft tissue volume, the prosthetic reduces the need for grafting.
We can achieve excellent aesthetics and function and provided we design the bridge appropriately; the patient has a high hygiene maintenance capability. It is a simple surgical prosthetic procedure for efficient treatments in terms of surgery type. However, for some patients a hybrid restoration is not the best idea. It is not always suitable for patients with a gummy smile. The interface between the bridge and the patient’s ridge must be above the patient’s lips and so patients with a gummy smile may require a lot of ablation (bone removal) to hide this interface.
Aggressive ablation particularly when in young patients may not always be in the patients best interest. Ablation will impact on the available bone for this procedure and for any further surgery required in the patient’s lifetime.
Similarly, some patients just don’t like the look of hybrid when shown an example.
An avid user and course tutor on the TeethXpress® immediate load protocol from BioHorizons Camlog, this system is ideal for fully or partially edentulous patients. Using a combination of the BioHorizons Tapered implant the TeethXpress® technique, creates a reliable predictable and efficient workflow, helping shorten treatment time, minimise chair time and ultimately maximise profitability.
Who is suitable for immediate full-arch treatment?
Patients suitable for immediate full arch treatment are the terminal perio patient, those who have failing large span bridges (often on posts), those that are unhappy removable partial denture wearers (and whose remaining teeth are of dubious prognosis) and the unhappy complete denture wearer. Each of these patients will have different aspects to consider.
With the terminal perio patient you need to ask yourself, “is this patient going to take our advice and improve their oral hygiene, both in the short and long term?” By nature, these patients are at a higher risk of peri-implantitis.
With patients who have a failing crown and bridge, it is important to be aware of root fractures which can mean very little bone is available for the implant placement. It’s also vital to eliminate any acute periapical abscess as you cannot place implants in sites acute to infection. Parafunction needs to considered too, as well as assessing the biotype.
With patients who have partial dentures, it is imperative to motivate the patients about the benefits of full arch implant treatment , as opposed to repeated episodes coming in for an extraction and another tooth added to the their increasingly unstable partial denture. In some cases, their existing teeth can provide the best implant sites and elective clearance simplifies the treatment. Hygiene improvement needs to be stressed for these patients and will be slightly more challenging with a fixed prosthetic.
With regards to complete denture wearers, it is difficult to assess parafunction. Therefore, before embarking on treatment, it is important to check lip support without the flange and assess the available bone and keratinised tissue in the mandible.
It’s very important, to demonstrate the bulk of the prosthesis to those patients who may have never worn a denture, so that they can see what we will be aiming for. Additionally, we have no idea how well patients will adapt to oral hygiene measures so they will require some education for additional motivation.
What are the key factors for full-arch success?
Initial stability is vital and allows for osseointegration under the functional load. The benefit of rigid cross arch splinting allows for immediate load. Where possible, reduce the grafting, as graftless surgery also equals less complications and anterior posterior spread is more important than the number of implants. It is essential to minimise the cantilever lengths and adequate restorative thickness for the prosthesis.
The number of implants required for full arch treatment will centre around bone quality, spaced anterior posterior spread, and our implant dimensions. So why would we place less implants? More implants can mean more potential for inaccuracy with impression taking and prosthesis, more implants and abutments for the patient to clean, and more holes in the bridge can weaken the structure.
Patient consent for full-arch rehabilitation
Since implant rehabilitation is an elective treatment, as clinicians we have a professional responsibility to support the patient in making an informed decision in accordance with both their medical history and their quality of life.
My advice is to always show the patient a model of what you can deliver and discuss the number of teeth you can achieve, based on planning and scans. Make sure you discuss the limitations and specific limiting factors before you start the procedure.
The best course of action is to send the patient a letter outlining the risks, benefits, and options, outlining the expectations of what will be happening. Standard protocol in any cosmetic medical procedure, I would also advise carrying out a psych assessment to ensure that the patient is ready for the treatment and has the support from their family.
The psychological impact of tooth loss shouldn’t be underestimated too. Poor appearance and function lead to poor self-esteem and loss of confidence. It is essential patients can cope with treatment and we encourage patients to bring a family member with them to consultations for support.
There may be several barriers to treatment acceptance – cost, fear and time. However, once you explain how life-changing this treatment can be, discuss finance and sedation options and how full-arch only takes a few appointments to achieve fantastic results, you may be well on the way to a positive outcome.
To hear more about my views and experience on full-arch treatment please take a look at the following:
- Webinar – Watch the full webinar here ‘Complete your implant practice with full-arch treatment’.
- Course – Attend my 2-day course ‘Immediate Loading with TeethXpress- Live surgical & restorative demonstration’.
- Event – I will be speaking at the BioHorizons Camlog UK & Ireland Symposium – Implants for life; a patient-centric approach to dental implantology in September 2022, around ‘Treatment options for longstanding success in full arch reconstruction’.
- Articles – More articles here:
For more information about BioHorizons Camlog products and solutions visit www.theimplantrevolution.co.uk or contact your local Territory Manager here.








