The rules and pitfalls of hard and soft tissue grafting

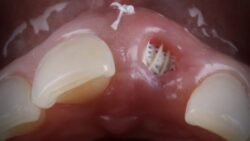
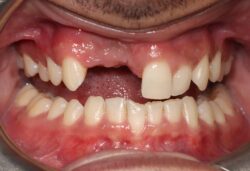
Dr Fazeela Khan-Osborne discusses the types of hard and soft tissue defects that commonly arise in implant dentistry and talks about common mistakes, the options available and the complications that may arise.
My vast experience in working in implant dentistry and educating GDPs all over the world over the past 25 years means that I am very familiar with the common mistakes made when diagnosing bone and soft tissue defects, the complications that can arise and how dentists can avoid them.
Firstly, we should always start from the treatment planning at the start with an assessment of the site. Sometimes it is a tooth that is failing and is yet to be removed. Other times it is a decision that we have to make that it’s a single space in the aesthetic zone or it can be a naturalised area that has been like that for some time. The criteria for the bone grafting and each of those two potential scenarios would be different. These are questions which we need to be asking at the assessment stage.
The main decision for criteria for immediate placement would be:
- Is the socket intact – with no vestibular, mesial, distal or palatal bone loss?
- No acute pathology?
- Are there acceptable soft tissue contours?
- Ensure that we are going to achieve acceptable aesthetics.
It’s also vital to consider.
- What happens to a socket when we extract teeth in the aesthetic zone?
- What are the common mistakes of diagnoses at the assessment phase?
- Does grafting the socket prevent buccal wall collapse that we often see in upper anterior teeth?
- Does immediate implant dentistry minimise buccal wall resorption?
- Does grafting the gap improve the implant survival for the long term?
What does bone augmentation seek to achieve?
The aim of bone augmentation is to reconstruct a deficient ridge to a form which will ensure that an aesthetic implant supported restoration can be constructed. In contrast, the aim of the soft tissue augmentation is to improve the functional and aesthetic outcomes where any compromise in soft tissue thickness or quantisation or even volume has occurred.
One of the mistakes that often occurs is that GDPs diagnose and treat according to their skill set. It’s vitally important for dentists that after the initial training, they move onto the advanced complex bone and soft tissue grafting procedures and courses that will allow them to treat the whole gamut of treatments that they may be presented with.
Often if the patient has had implants already, you will have a bone defect and therefore having these skills to carry out hard and soft tissue augmentation is essential going forward.
The treatment options that are available to us for deficient bony ridges tend to be of three main types: an onlay graft, an interpositional graft and a particulate (containment, mesh or membrane, staged).
What are our grafting aims and considerations?
Before grafting is considered, the long-term criteria and concepts that we need for success in implant dentistry for our restorations must be deliberated. We need to marry that with options for hard and soft tissue grafting that are available to us and look at any complications that may arise – i.e. flap design, infection, or graft shrinkage, and their corrections as well as the role of extraction socket therapies.
Things to consider before placing an implant:
- Bone grafting
- One or two stage surgery
- Autogenous blocks vs allografts
- Ridge preservation techniques
- Blood supply to the bone graft and soft tissue
- The aesthetic zone
- Preservation of papilla soft tissue thickness
- Bone graft procedures and soft tissue thickness.
Each of these assessment factors are vital, culminating in your diagnosis and final treatment plan. When looking at the key factors for long term success, the three fundamental areas are; bone, soft tissue thickness, and attached gingiva.
In addition to your assessment of the patient and the area that is going to receive the implant, you must also carry out planning on your CT scan. Look at the height and width, the position of anatomical features, such as the ID canal or the mental nerve, the sinus floor and in the aesthetic zone looking at the thickness of the patient or buccal plate. Your surgery can then be pilot guided or fully guided and depending on the amount of height and width you have, it will also guide you to the density and the drilling sequence that you might use – whether it’s healed ridge or an immediate site.
Defect shape and graft suitability
When considering hard and soft tissue grafting techniques, there is a dependency on the size and shape of the defect, and how many walls are affected. The graph stability will also depend on the most suitable graph being chosen to match the defect. This will be dependent on the type of graft and the type of defect, as well as how long that edentulous area has been there.
If we look at it according to this methodology, we will be looking at the hardened tissue graft options that are available to us. Therefore, if we go from the most minor ridge or socket augmentation, through the immediate placement grafting the gap through to guided bone regeneration including the Sausage Technique (Urban), to bone blocks such as MinerOss® allograft block, and finally PET therapies – this really forms the mainstream of the hard tissue grafting options which we have available.
Ultimately, the role of the regional augmentation or the socket preservation is to try to modulate and minimise the amount of contour change that will take place and to hold the contour of the hard tissue and soft tissue while also encouraging new bone to form prior to your implant placement.
Ridge preservation techniques and guided bone regeneration
Ridge preservation techniques do not stop bone resorption or bone loss per se, but it can reduce the degree of socket dimensional change. The materials most commonly used are autograft, allograft (such as MinerOss® Blend) and xenograft (such as MinerOss® X). The primary wound closure is an important factor with either the use of a type one collagen membrane (such as Mem-Lok®), or to use a connective tissue graft which is autogenous, which would also add to the thickness and volume of the soft tissue.
The aims of indications for GBR is to preserve the reach during the healing phase, to augment any deficient ridges, and to fill in defects around immediately placed implants by grafting the gap and to treat bony defects. The factors that affect the success of this is the consistent and good packing of the particulate material, the immobility of the barrier membrane, absence of wound dehiscence and associated infections, and adequate healing time.
Connective tissue grafting
With connective tissue grafting, it is important to make sure you don’t have a bleed, post-op pain or infection from the harvest donor site. With all grafts, it is essential to fix and have an intimate apposition of the graft to the host bed, to allow good fixation containment of the graft and full primary closure where possible and graft immobility to allow the reestablishment of the blood supply, and ultimately the success of your hard or soft tissue graft.
Taking this into consideration, the indications with the free gingival graft is to increase keratinised tissue and thickness and height around teeth implants and crowns, and to increase the vestibular debt.
To conclude…
Although bone grafting can be daunting, our courses are specifically developed to include live surgery with both soft and hard tissues and also give delegates the opportunity to produce cases themselves. Many dentists misdiagnose in this discipline, and it can be quite overwhelming – my advice is to get in touch with your peers and established educators who can help you move onto the next stage of your career.