Standing on the shoulders of biologic scaffolds

Read on to discover the science behind bone grafting, trends and market growth, and the difference between allograft and xenograft materials.
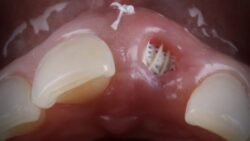
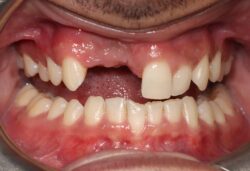
Due to the growing demand for transformative implant treatment, bone grafting has become commonplace in dentistry as sufficient bone volume and quality is necessary for successful placement of the implants. Proper treatment planning for bone graft placement requires the clinician to select the appropriate surgical technique and product because poor execution could lead to resorption of the graft material.
The advent of modern bone grafting technology means soft and hard tissue limitations are a thing of the past. For those looking to grow their implant patient base, considering the practical advantages of using biologic scaffolds in your edentulous cases is a must. Plus with such a comprehensive scope of biologics solutions available on the market today, it’s important clinicians feel confident in choosing the material that’s right for them, the treatment and ultimately the patient.
Filling in the gaps of bone and tissue regeneration
Market growth: The global dental bone and graft substitute market size is estimated to reach USD 719.1 million in 2021 and is expected to grow at a CAGR of 11.4% from 2021 to 2028i. Europe is dominating this market with a share of 39% in 2019ii. Key growth factors include a rising geriatric population, an increasing number of tooth disorders and extractions, and the growing importance of aesthetics and quality of life with implants amongst our ‘commercially aware’ patients.
Applications: A common procedure across many medical disciplines, bone grafts are used as a filler to promote healing and act as a mineral reservoir to facilitate new bone growth. Whilst the increased burden of poor dental conditions saw socket preservation applications hold the highest market share in 2020 (29%)iii, the increasing demand for implant treatment will further propel the application of ridge augmentation procedures. Helping to recreate the natural contour of the gums and jaw, support dental implants, quick recovery and painless procedures are all contributing factors to estimating this as the fastest-growing application over the next eight years.
Materials: Generally, the market is segmented into allograft, autograft, xenograft and synthetic materials. Historically, practitioners utilised synthetic grafting materials which often triggered inflammatory responses and demonstrated limited biocompatibility in the patient. Modern grafting procedures make use of more appropriate material i.e., biological tissue sourced from the patient (autografts), animal (xenografts) or human (allografts) donors. As a biologic scaffold, bone grafts are inherently bioresorbable and have no antigen-antibody reaction. These naturally occurring matrices encourage stem/progenitor cell regeneration at the site of remodelling, and therefore, act as an effective accelerant of new tissue growth (Costa et al.,2017)iv.
Allografts versus Xenografts
Limited tissue availability and the harvesting process’s potential morbidity factor have pushed dental practitioners to seek innovation in regenerative technology. Whilst traditional autogenous grafts have served the implant surgeons purpose well, alternatives such as allografts and xenografts provide similar results whilst avoiding a second intraoral wound.
Allografts are biologic tissues derived from human donors and typically sourced from a bone bank. The externally sourced donor tissue undergoes an extensive cleaning process to remove blood and tissue components, eliminate fat and deactivate proteins from the cancellous and cortical bone structure which helps to improve penetration of the surrounding tissue into the grafting material.
From demineralised matrix granules to complete bone segments, allografts are available in a wide range of sizes depending on the treatment e.g., socket preservation for future implant placement, filling osseous defects, maxillary sinus floor elevation and ridge reconstruction.
Accounting for the largest market share in 2020 (47%), xenografts, on the other hand, are derived from a different species, or organisms, such as bovine or porcine. As porous natural hydroxyapatite can be obtained from animal bones, xenografts are successful in stimulating bone tissue morphology to provide long-term stability. With a long-standing and well-documented history in grafting, bovine bone grafts are prepared and deproteinised through heat, eliminating the risk of disease transmission and allergic reaction. Removing existing protein transforms the bone into a hydroxyapatite ceramic characterised by a well-preserved 3D bone structure very similar to human bone (Goldstep, 2015)v.
The xenografts trabecular architecture and interconnecting pores allows for optimal new vascularity in-growth and leads to exceptional volume stability for new bone formation. Similar to allografts, xenografts are osteoconductive and are available in a range of particle sizes and volumes (Sousa et al., 2013)vi.
Biologic Solutions
Whichever grafting solution you choose, you need to feel confident and empowered to use the scaffold material to its full potential. If you’re looking for a comprehensive line of hard tissue products to support bone grafting procedures of all sizes, choose the MinerOss family of bone grafting solutions.
With comprehensive literature, representative support, courses and on-demand webinars at your disposal, you can discover the freedom to regenerate with biologics. Learn more here.